The coronavirus or SARS-CoV-2 as its medically known isn’t the only viral disease to ever plague the human race. Despite so many of them, there are some that are extremely dangerous and deadly while there are others that aren’t so.
The development of vaccines have also been a great thing that has kept these viruses at bay. From deadly diseases like smallpox to measles both of which had ravaged the earth in the not-so-long past to the recent COVID-19 pandemic and other series of diseases that have been listed to the disease book of the World Health Organization.
But the battle is long from ending but thanks to modern medicines and the discovery of vaccines, humans have been able to persist and fight against these deadly pathogens.
One of the most challenging situations scientists have found themselves in is the fact that some pathogens are able to jump from their host usually other species of animals to the human species where they then mutate and cause series of havoc.
Ebola virus is one of such which has a very high mortality rate killing about 90% of those that have the disease is said to have come from bats which is the natural reservoir.
But that’s not the only virus. There are some that humans have been able to keep at bay which if they lead to a pandemic could wipe a large number of the human population out just like the time of the Black Death or the Spanish Flu.
Here are the 12 worst killers, based on the likelihood that a person will die if they are infected with one of them, the sheer numbers of people they have killed, and whether they represent a growing threat.
The Marburg virus
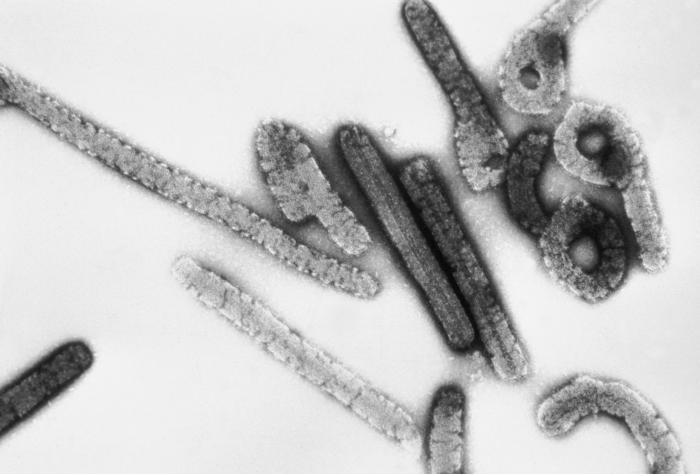
The Marburg virus was first discovered by scientists back in the year 1967 due to a small outbreak in a laboratory in Germany because they were exposed to infected monkeys that were imported from Uganda.
The Marburg is said to be closely similar to the Ebola virus in that they both cause hemorrhagic fever – a severely high fever and bleeding throughout the body that can cause shock, organ failure and death
The mortality rate in the first outbreak was 25%, but it was more than 80% in the 1998-2000 outbreak in the Democratic Republic of Congo, as well as in the 2005 outbreak in Angola, according to the World Health Organization (WHO).
Ebola virus

The 2014 outbreak of the Ebola virus isn’t the first occurrence of the deadly disease as there had been a recorded occurrence back in the Republic of the Sudan and Democratic Republic of Congo back in the year 1976.
The disease spread when a human come in contact with blood or other body fluids or tissue from an infected person or animal.
The known strains vary dramatically in their deadliness, Elke Muhlberger, an Ebola virus expert and associate professor of microbiology at Boston University, told Live Science.
One strain, Ebola Reston, doesn’t even make people sick. But for the Bundibugyo strain, the fatality rate is up to 50%, and it is up to 71% for the Sudan strain, according to WHO.
The 2014 outbreak in West Africa was the largest and most complex of the disease to date according to the WHO.
The outbreak underway in West Africa began in early 2014, and is the largest and most complex outbreak of the disease to date, according to WHO.
Rabies
Thanks to scientists, there are now anti-rabies for pets such as dogs which were introduced back in 1920s and is available around the world. Vaccines have helped to reduce the rate of rabies especially in developed countries.
But this condition is still common in developing regions of the world especially Africa and India. “It destroys the brain, it’s a really, really bad disease,” Muhlberger said.
“We have a vaccine against rabies, and we have antibodies that work against rabies, so if someone gets bitten by a rabid animal we can treat this person,” she said.
However, she said, “if you don’t get treatment, there’s a 100% possibility you will die.”
HIV

HIV is still one of the most complicated disease in modern history with many questioning why its yet to get a cure and others formulating their own conspiracy theory about the disease being used for political gains and so forth.
“It is still the one that is the biggest killer,” said Dr. Amesh Adalja, an infectious disease physician and spokesman for the Infectious Disease Society of America.
Since it was first documented back in the 1980s, the disease is said to have killed about 32 million people worldwide “The infectious disease that takes the biggest toll on mankind right now is HIV,” Adalja said.
However there have been some powerful antiviral drugs which has made it possible for those living with the disease to have their life to the fullest.
But the disease continues to devastate many low- and middle-income countries, where 95% of new HIV infections occur. Nearly 1 in every 25 adults within the WHO African region is HIV-positive, accounting for more than two-thirds of the people living with HIV worldwide.
Smallpox

For the first time in 1980, the WHA or World Health Assembly declared the world free of Smallpox. This was a breakthrough in medicine considering the devastating effects this disease has caused for thousands of years in the human specie.
Smallpox was so deadly it would kill 1 in 3 person that has it and even those that survived would be left with horrible scars for the rest of their lives such as blindness.
Mortality rates were far higher in populations outside of Europe, where people had little contact with the virus before visitors brought it to their regions. For example, historians estimate 90% of the native population of the Americas died from smallpox introduced by European explorers. In the 20th century alone, smallpox killed 300 million people.
“It was something that had a huge burden on the planet, not just death but also blindness, and that’s what spurred the campaign to eradicate from the Earth,” Adalja said.
Hantavirus

There were rumors about the Hantavirus back in 2020 during the COVID-19 pandemic. The HPS or Hantavirus Pulmonary Syndrome gained its notoriety in the US when a healthy, young Navajo man and his fiancée living in the Four Corners area of the United States died within days of developing shortness of breath. A few months later, health authorities isolated hantavirus from a deer mouse living in the home of one of the infected people.
More than 600 people in the United States have contracted the HPS with 36% of them dying from the disease according to the Centers for Disease Control and Prevention (CDC)
While the HPS isn’t communicable from one person to the other, the disease is often due to being exposed to droplets from infected mice.
Previously, a different hantavirus caused an outbreak in the early 1950s, during the Korean War, according to a 2010 paper in the journal Clinical Microbiology Reviews. More than 3,000 troops became infected, and about 12% of them died.
While the virus was new to Western medicine when it was discovered in the U.S., researchers realized later that Navajo medical traditions describe a similar illness, and linked the disease to mice.
Influenza

According to the World Heath Organization, during a flu season, about 500,000 people around the world will die from the disease. There are usually situations when a new flu strain emerge or a pandemic which spread faster, this increases the mortality rates.
The most deadly flu pandemic, sometimes called the Spanish flu, began in 1918 and sickened up to 40% of the world’s population, killing an estimated 50 million people.
“I think that it is possible that something like the 1918 flu outbreak could occur again,” Muhlberger said. “If a new influenza strain found its way in the human population, and could be transmitted easily between humans, and caused severe illness, we would have a big problem.”
Dengue

Dengue virus was first documented in the 1950s after it appeared in the Philippines and Thailand and has spread across the tropical and subtropical regions of the globe.
Up to 40% of the world’s population now lives in areas where dengue is endemic, and the disease — with the mosquitoes that carry it — is likely to spread farther as the world warms.
The dengue virus is aid to affect about 50 to 100 million of people every year according to the WHO but the mortality rate is far lower compared to other viruses on this list.
In contrast, Dengue virus has 2.5% mortality compared to the likes of Ebola virus which could reach 70%. The disease is also Ebola-like in its symptoms as it causes hemorrhagic fever which could increase the mortality to 20% if left untreated.
“We really need to think more about dengue virus because it is a real threat to us,” Muhlberger said.
Not until 2019 did we get vaccine approved to combat the Dengue virus by the FDA for use in children between the age of 9 and 16 and living in areas where the disease is very common and with a confirmed history of virus infection.
In some countries, an approved vaccine is available for those 9-45 years old, but again, recipients must have contracted a confirmed case of dengue in the past. Those who have not caught the virus before could be put at risk of developing severe dengue if given the vaccine.
Rotavirus
Advertisement

Scientists have been able to manufacturer about two different vaccines to protect children from the dangerous Rotavirus which causes severe diarrhea among babies and young children.
The virus can spread rapidly, through what researchers call the fecal-oral route (meaning that small particles of feces end up being consumed).
Although children in the developed world rarely die from rotavirus infection, the disease is a killer in the developing world, where rehydration treatments are not widely available.
According to the World Health Organization, there are over 453,000 deaths in children under the age of 5 in the year 2008. But countries that have introduced the vaccine have reported sharp declines in rotavirus hospitalizations and deaths.
SARS-CoV
Advertisement

The SARS-CoV is the disease that causes the Severe Acute Respiratory Syndrome or SARS which was first reported back in the year 2002 in China according to the WHO.
The origin of the disease has been linked to bats as being the natural reservoirs and the outbreak has spread to about 26 countries worldwide with over 8000 reported cases of infections and 770 deaths.
Symptoms of SARS includes high fever, chills and body aches which often progress to pneumonia, a state where the lungs become inflamed and ridden with pus.
SARS has an estimated mortality rate of 9.6%, and as of yet, has no approved treatment or vaccine. However, no new cases of SARS have been reported since the early 2000s, according to the CDC.
SARS-CoV-2
The current SARS-CoV-2 belongs to the family of the SARS-CoV or the Coronaviruses. And the SARS-CoV-2 was reported in the year 2019 after it has reportedly jumped from bat to human in China.
The disease has since affected millions across the world and was declared a pandemic in 2020 with more than a million fatal cases worldwide.
The disease caused by SARS-CoV-2, called COVID-19, has an estimated mortality rate of about 2.3%. People who are older or have underlying health conditions seem to be most at risk of having severe disease or complications. Common symptoms include fever, dry cough and shortness of breath, and the disease can progress to pneumonia in severe cases.
MERS-CoV

The MERS-CoV or Middle East Respiratory Syndrome is also a member of the Coronavirus whose 2012 outbreak caused global concerns. There was another outbreak in South Korea 3 years later.
The MERS virus belongs to the same family of viruses as SARS-CoV and SARS-CoV-2, and likely originated in bats, as well. The disease infected camels before passing into humans and triggers fever, coughing and shortness of breath in infected people.
MERS often progresses to severe pneumonia and has an estimated mortality rate between 30% and 40%, making it the most lethal of the known coronaviruses that jumped from animals to people. As with SARS-CoV and SARS-CoV-2, MERS has no approved treatments or vaccine.



